For patients with advanced kidney disease, transplantation offers far more than an alternative to dialysis — it offers the chance to live longer, feel better and reclaim a full, active life.

“Every day, we see patients whose lives could be transformed by a kidney transplant,” said WashU Medicine – Department of Medicine transplant Nephrologist Dr. Tarek Alhamad. “Our goal is not just survival, but restoring quality of life.”
At WashU Medicine, the kidney transplant program continues to grow steadily, with a target of performing approximately 400 transplants annually by 2027. Increased referrals and evaluations reflect both rising need and expanding awareness of transplantation as the optimal treatment for end-stage kidney disease.
Early Referral Makes a Life-Changing Difference
Patients qualify for kidney transplantation when they develop advanced chronic kidney disease or require dialysis. Yet many patients are referred too late — often after spending years on dialysis — despite clear evidence that earlier referral leads to better outcomes.
“The ideal scenario is preemptive transplantation — receiving a kidney before dialysis is ever needed,” Dr. Alhamad explained. “Dialysis is physically and emotionally exhausting. If we can avoid it altogether, we should.”
Referrals can come from nephrologists, dialysis providers, nurses, social workers or directly from patients themselves. The program accepts all referral pathways, emphasizing accessibility and early engagement.
The Silent Nature of Kidney Disease
Kidney disease is often called a “silent disease” because it typically causes no symptoms until significant damage has already occurred. Diabetes and hypertension remain the leading causes, accounting for nearly two-thirds of cases nationwide.
“People may feel completely fine while their kidney function quietly declines,” said Dr. Alhamad. “By the time symptoms like swelling, fatigue or shortness of breath appear, the damage has usually been ongoing for years.”
This underscores the importance of regular medical follow-up, blood pressure control and diabetes management — particularly in communities disproportionately affected by kidney disease.
Dialysis vs Treatment
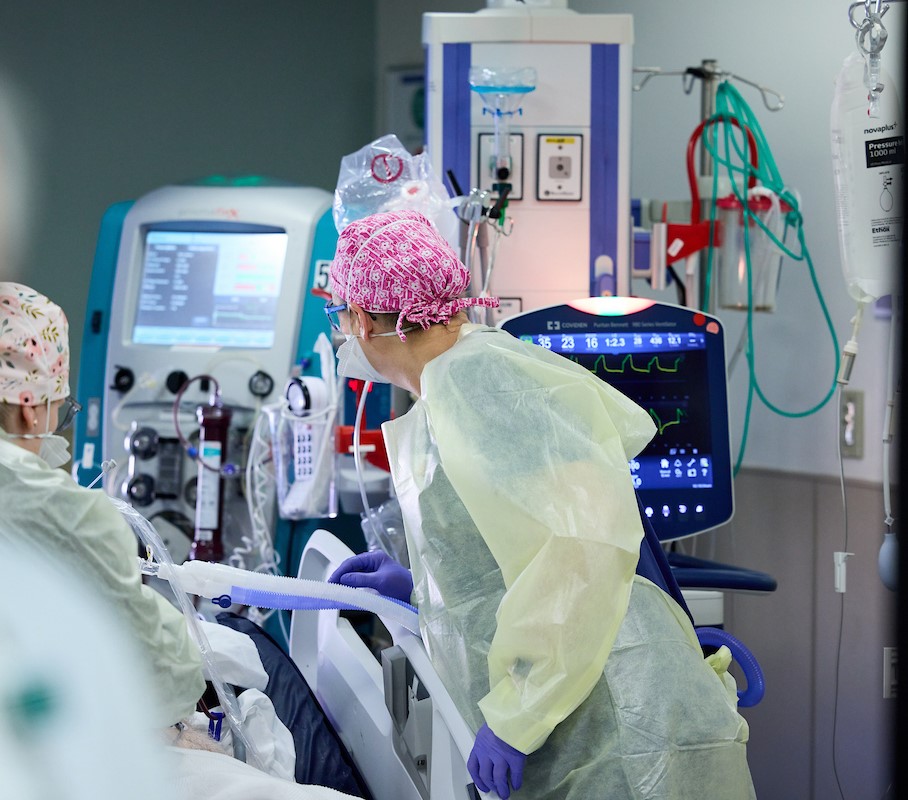
While dialysis sustains life, it often comes at a steep cost. Patients typically spend three to four days each week connected to machines for hours at a time, experiencing fatigue, weakness and diminished independence. Depression is common, and many patients are unable to work, travel or fully participate in family life. Kidney transplantation offers a different future.
“After transplant, patients often tell us they feel better than they have in years,” Dr. Alhamad said. “They return to work, travel, spend time with family — and young women can safely conceive and carry pregnancies again.”
One Kidney is Enough and Living Donation Saves Lives
Only one kidney is needed to sustain normal function. A transplanted kidney from a deceased donor lasts an average of 12 years, while a kidney from a living donor often functions 15 to 17 years or longer.
Living donation offers multiple advantages: shorter wait times, better matching, lower rejection risk and significantly longer graft survival. Donors themselves face minimal long-term risk, with studies showing their chance of developing advanced kidney disease is comparable to the general population.
“Living donation gives recipients more years of life — and gives donors the extraordinary opportunity to save a life,”
– Alhamad
Despite these benefits, living donation rates remain lower in some regions. The transplant team continues to expand education efforts, helping patients learn how to share their stories, use social media and engage broader networks to find potential donors.
“We are often amazed by people’s generosity,” Dr. Alhamad added. “Some donors step forward simply because they want to help. They truly give the gift of life.”
Overcoming Barriers and Misconceptions
Fear and misinformation still prevent some patients and families from pursuing transplantation or donation. Common misconceptions include fears about donor safety, confusion about transplant medications and mistrust rooted in historical inequities.
“Transplant is not experimental, and immunosuppressive medications are not chemotherapy,” Dr. Alhamad emphasized. “While there are risks of possible complications of side-effects, patients live longer and better lives compared to remaining on dialysis.”
Education remains a cornerstone of the program — for patients, families and frontline dialysis providers alike.
Expanding Access Through Outreach
As the largest kidney transplant center in Missouri, WashU Medicine actively reaches beyond the St. Louis region to improve access to transplantation. Outreach efforts include provider education, community visits and partnerships across Missouri, Illinois, Arkansas, Iowa and Kentucky.
“These conversations change practice,” said Dr. Alhamad. “When providers see the outcomes, referrals increase — and patients benefit.”
For Dr. Alhamad and the transplant team, the work is deeply fulfilling.

“It takes a village — nephrologists, surgeons, coordinators, nurses, social workers, HLA lab staff, pathologists — everyone plays a role,” he said. “Seeing a patient come off dialysis and return to life is one of the most rewarding experiences in medicine.”
As research continues into new therapies and future options such as xenotransplantation, the message remains clear: kidney transplantation saves lives — and organ donation makes it possible. Learn more about Dr. Tarek Alhamad and follow him on X @TransplantPulse
Careers in Nephrology
If you’re interested in advancing your career in nephrology and transplantation, we encourage you to explore the WashU Medicine Nephrology Transplant Fellowship program. Visit their website to discover more about the comprehensive training, cutting-edge research opportunities, and exceptional clinical experiences that our program offers. Join WashU Medicine to become a part of a leading institution dedicated to innovation and excellence in healthcare.